Sickening: How Big Pharma Broke American Health Care and How We Can Repair It
By John Abramson
Mariner
Ethically Challenged: Private Equity Storms US Health Care
By Laura Katz Olson
Johns Hopkins University Press
The coronavirus pandemic has laid bare major systemic problems in the U.S., nowhere more than in the cruelty and irrationality of our for-profit health care system. Even though we spend 19.7 percent of GDP each year on health care (about $4.5 trillion), 11 other wealthy countries spend just over 10 percent and often deliver better results. The U.S. ranks 69th in the world when judged on “healthy life expectancy,” and for the first time in decades, American life spans dropped from 2014 to 2018.
Two new books pry even deeper into our dysfunctional health care system. One looks at the way that pharmaceutical companies exert enormous influence on the design, conduct, and analysis of clinical research. The other examines how private equity (PE) firms have lately been acquiring and streamlining health care companies in a way that siphons supersized profits for themselves, but undermines the right of all other Americans to have access to affordable, timely, and high-quality care.
In Sickening: How Big Pharma Broke American Health Care and How We Can Repair It, John Abramson, a lecturer at Harvard Medical School, points out that over the past four decades, “the pharmaceutical industry has been able to achieve ‘tail wags dog’ position” to tilt the playing field in its favor, at great cost to patients. Its ruses include funding studies about its own drugs; distorting clinical trial data to increase drug sales; delaying publication of economically inconvenient findings; buying reprints of articles in prestigious medical journals; cultivating relationships with doctors; running dubious ads; and more. The industry has also spent at least 50 percent more on lobbying since 1998 than any other individual sector.
Abramson draws from 22 years of experience as a family physician, a consultant to the Department of Justice, and an expert witness in several trials involving pharmaceutical companies. His book brims with arcana, from the Food and Drug Administration’s flawed approval process for drugs (and loopholes like the “501(k) pathway” for certain medical devices), to the problem with passing off post hoc findings as primary ones, to the need for an independent federal health board, something with support from lawmakers in both parties.
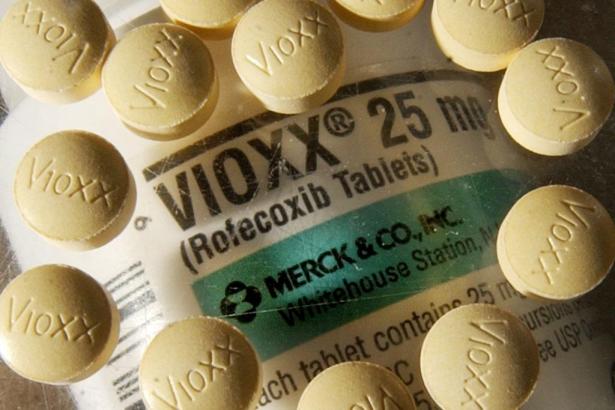
One individual he writes about was prescribed Vioxx (“a safer version of ibuprofen”) for pain relief, only to experience debilitating headaches and eventually death from a massive stroke. “If it weren’t for the failure of three guardians of public safety,” Abramson writes, the death could have been prevented. Merck, the manufacturer, had concealed Vioxx’s increased cardiovascular risk. The New England Journal of Medicine had published an article claiming the drug was safe to use, and failed to update readers when it learned about the risk until five years later. And the FDA dragged its feet when it came to acting on the risks.
Each of these malefactors—the FDA, medical journals, and drug manufacturers—come under closer scrutiny in subsequent sections. Pfizer, which has lately benefited from a pandemic halo, is singled out for its role in an illegal off-label-marketing scheme involving Neurontin, a drug that had been approved by the FDA to treat epilepsy and a specific type of nerve pain. Abramson was an expert witness in the Neurontin case, where he explained Pfizer’s “statistical shenanigans,” including a “continuing medical education” meeting for doctors that presented favorable-looking results for only 15 patients, with no control group or comparison drug study.
The jury concluded that Pfizer had fraudulently marketed Neurontin to doctors, but the penalty it paid ($142 million) amounted to “less than half the revenues from one year of Neurontin sales.” Abramson was personally and professionally disheartened at the modus operandi for companies like Pfizer: “Under our current system, it is more profitable for large pharmaceutical companies to commit crimes and pay the fines than to obey the law.”
Abramson notes that standing up to Big Pharma and rapacious insurance companies and hospitals will require “a coalition of health-care professionals, purchasers (including non-health-care-related businesses, unions, and governments), and consumers.” But his call to “find a better balance between commercial profit and public benefit” is too equivocal by half, stopping well short of an overhaul of the system. One-third of the billions raised on GoFundMe is for essential medical services. Working out the mean between profit and the public interest would be like solving the SAT problem from hell. Every other industrialized country has figured out that a Medicare for All–style system allowing the government to negotiate for more affordable drugs would prevent consumer price-gouging, which Big Pharma has reliably done year after year despite national outcry.
However, this does not seriously mar a riveting, insider’s account of the medical guild, with its influential medical journals, clinical practice guidelines, and, inescapably, an avalanche of “expertly developed commercial propaganda, and, sometimes, simply lies.”
ABRAMSON WRITES THAT, STARTING AROUND 1980, “Companies moved from addressing the needs of a broad array of stakeholders … to focusing narrowly on maximizing financial return to shareholders.” This is about the same time that private equity firms began flourishing by breaking up public companies in the pursuit of profit. Abramson briefly gestures at the disemboweling of the welfare state and neoliberalism’s sculpting of the U.S. political economy to favor privatization, but he leaves out any mention of PE firms, whose buyouts have sprouted up in several health care sectors with rank luxuriance, valued at dozens of billions of dollars each year.
Private equity is largely responsible for the phenomenon of balance (or surprise) billing, which can ensnare patients who have health insurance but are treated by an out-of-network medical professional, like a physician in an emergency room who works for a third-party physician staffing company. Putting Americans in debt from surprise medical bills is nearly universally despised, yet, as Laura Katz Olson shows in her important and revealing new book Ethically Challenged: Private Equity Storms US Health Care, it’s a practice that became increasingly common after PE firms started taking over medical companies.
At the molten core of the private equity business model is the practice of accruing massive piles of debt to make investments, and requiring the companies they buy to pay it off. Drawing largely from state and local pension funds and endowments, private equity “is neoliberalism on steroids,” writes Olson. “Supersized earnings for PE and its shareholders are front and center, with no pretense otherwise.” The fact that it is accountable to no one other than its investors means that a great deal of its financial transactions are fogged in mystery.
Private equity has begun to consolidate segments of U.S. health care, at the expense of patients and workers.
Constantly selling off assets of a current buyout to finance future conquests, PE firms are a bit like the mythical ship of Theseus, forever being reconfigured with new parts—if Theseus were a plutocrat with a passion for dividend recapitalizations. Adding to the atmosphere of omertà, erstwhile founder-owners who saw their practices acquired by PE and who were willing to be interviewed for Olson’s book could only disclose so much without running afoul of nondisclosure agreements. Still, there’s enough data for Olson to make a convincing case that PE has infiltrated almost all imaginable recesses of our lives, from the way we communicate to where we shop for groceries to how we charge our electronic widgets to—most worrying of all—where we get treated for medical emergencies or drug addiction.
Specialized establishments like home care and hospice centers, diagnostic labs and imaging centers, pharmaceutical companies, medical device businesses, dialysis facilities, fertility clinics, urgent care centers, and dermatologist offices have all been swallowed up by PE. Since 2011, reports Olson, the trend in many of these health sectors has been add-ons and mergers, with PE houses bundling acquisitions to “achieve scale” and “expand geographic reach” rather than selling off parts. According to Axios, in 2018 alone, there were nearly 800 private equity health care deals, nearly 15 percent of all PE acquisitions, yielding a total value of more than $100 billion.
It’s not uncommon for PE-held hospitals to pressure physicians to maximize “patient volume,” or to restrict the time they can spend with each patient, bilking people of proper care and attention. After Hospital Corporation of America was purchased by Bain Capital, KKR, and Merrill Lynch Global Private Equity in 2006, for instance, HCA engaged in a number of shady practices, including manipulating ER billing codes and turning away patients who failed to pay in advance. Physicians in other PE-owned firms have been found to “hard-sell products and treatments (some of which may be unnecessary), and be parsimonious with medical and other supplies,” writes Olson. Managing directors are “not particularly concerned” about their acquisition’s long-term viability or performance; what interests them most is the quickest route to windfall profits.
PE-owned firms frequently put up a facade of catering to patients’ consumer preferences, through accoutrements like telemedicine and remote patient monitoring. Yet they often skimp on less tangible aspects of care, such as substituting lesser-trained practitioners for more expensive physicians. As both Abramson and Olson point out, the very notion of “choice” in the context of health care is misleading: Patients rarely have a full picture of fees and are not positioned to “shop around” for services in an emergency as if choosing shoes. It would be more accurate to say that patients are not so much granted unfettered access to health care options as they are themselves instrumentalized, their health subordinated to profit motives.

Reps. Richard Neal (D-MA) and Kevin Brady (R-TX) initially frustrated efforts to rein in surprise medical billing.
PE has begun to consolidate segments of U.S. health care that lack clinical standardization and government oversight, such as eating disorder centers and autism treatment facilities. This allows owners to impose all sorts of cost-cutting and so-called “efficiency” standards at the expense of patients. Workers at such enterprises also suffer under PE’s ruthless calculus: They often experience crushing workloads, earn lower wages than at comparable non-PE outfits, and have fewer benefits as PE focuses on retrenching operating expenses. Olson cites a study that shows that PE-controlled shops were responsible for over 1.3 million job losses since 2009. When bankruptcies hit companies, workers bear the brunt of the impact, while general partners sail off with golden parachutes.
Upton Sinclair once wrote, “It is difficult to get a man to understand something when his salary depends upon his not understanding it.” As recently as 2019, the leadership of the House Ways and Means Committee, chair Rep. Richard Neal (D-MA) and ranking member Rep. Kevin Brady (R-TX), were intent on not understanding the need to protect unsuspecting patients from surprise medical bills. This was no surprise: Neal and Brady were bankrolled by the Blackstone Group and Welsh, Carson, Anderson & Stowe (WCAS), respectively, two private equity firms that own health care staffing companies. Though Olson declines to provide precise figures in her book, a report from Public Citizen reveals that in 2019 alone—when congressional leaders started cottoning on to the outsized earnings flowing into PE coffers—employees or political action committees connected to Blackstone and WCAS contributed $63,600 to Brady and $32,700 to Neal. Private equity–backed groups like Doctor Patient Unity also spent millions of dollars on fear-mongering ad campaigns painting a dystopian future if providers are restricted to charging market rates for their services.
The good news is that Congress did pass legislation, which then-President Trump signed into law, protecting patients from being socked with surprise bills from out-of-network staffing companies and emergency air transit. The bad news—for everyone but PE’s financial puppeteers—is that the bill does not apply to public payers, and ground ambulances are also exempt, meaning sick and vulnerable people can still pay punitively high fees for out-of-network transport.
Private equity buyouts have been facing increasing scrutiny on Capitol Hill since the bankruptcy of stores like Toys ‘R’ Us and the outcry over surprise billing. As PE scoops up more and more physician practices, with a perennial aim of double-digit returns, their pecuniary incentives will increasingly collide with the only thing that should matter: the health needs of patients. Call it the “Hypocritic Oath”: Their commitment is to making money hand over fist.
To rein in PE’s pernicious influence on health care, Olson calls for the removal of tax havens that enable its revenue-seeking behaviors and investing more in social services. Like Abramson, she thinks we currently spend too much on downstream health care costs and not enough on upstream non-medical-care determinants of health. There is too much at stake to stand idly by as PE titans amalgamate even more health and medical services—the lives of disabled, sick, elderly, and other vulnerable people depend on putting an end to the rapaciousness of corporate medicine.

Spread the word