It begins with a mild fever and malaise, followed by a painful cough and shortness of breath. The infection prospers in crowds, spreading to people in close reach. Containing an outbreak requires contact tracing, as well as isolation and treatment of the sick for weeks or months.
This insidious disease has touched every part of the globe. It is tuberculosis, the biggest infectious-disease killer worldwide, claiming 1.5 million lives each year.
Until this year, TB and its deadly allies, H.I.V. and malaria, were on the run. The toll from each disease over the previous decade was at its nadir in 2018, the last year for which data are available.
Yet now, as the coronavirus pandemic spreads around the world, consuming global health resources, these perennially neglected adversaries are making a comeback.
“Covid-19 risks derailing all our efforts and taking us back to where we were 20 years ago,” said Dr. Pedro L. Alonso, the director of the World Health Organization’s global malaria program.
It’s not just that the coronavirus has diverted scientific attention from TB, H.I.V. and malaria. The lockdowns, particularly across parts of Africa, Asia and Latin America, have raised insurmountable barriers to patients who must travel to obtain diagnoses or drugs, according to interviews with more than two dozen public health officials, doctors and patients worldwide.
Fear of the coronavirus and the shuttering of clinics have kept away many patients struggling with H.I.V., TB and malaria, while restrictions on air and sea travel have severely limited delivery of medications to the hardest-hit regions.
About 80 percent of tuberculosis, H.I.V. and malaria programs worldwide have reported disruptions in services, and one in four people living with H.I.V. have reported problems with gaining access to medications, according to U.N. AIDS. Interruptions or delays in treatment may lead to drug resistance, already a formidable problem in many countries.

Benin was the first country in West Africa to distribute mosquito nets to prevent malaria despite the pandemic.Credit...Yanick Folly/Agence France-Presse — Getty Images
In India, home to about 27 percent of the world’s TB cases, diagnoses have dropped by nearly 75 percent since the pandemic began. In Russia, H.I.V. clinics have been repurposed for coronavirus testing.
Malaria season has begun in Africa, which has 90 percent of malaria deaths in the world, but the normal strategies for prevention — distribution of insecticide-treated bed nets and spraying with pesticides — have been curtailed because of lockdowns.
According to one estimate, a three-month lockdown across different parts of the world and a gradual return to normal over 10 months could result in an additional 6.3 million cases of tuberculosis and 1.4 million deaths from it.
A six-month disruption of antiretroviral therapy may lead to more than 500,000 additional deaths from illnesses related to H.I.V., according to the W.H.O. Another model by the W.H.O. predicted that in the worst-case scenario, deaths from malaria could double to 770,000 per year.
Several public health experts, some close to tears, warned that if the current trends continue, the coronavirus is likely to set back years, perhaps decades, of painstaking progress against TB, H.I.V. and malaria.
The Global Fund, a public-private partnership to fight these diseases, estimates that mitigating this damage will require at least $28.5 billion, a sum that is unlikely to materialize.
Delays in diagnosis
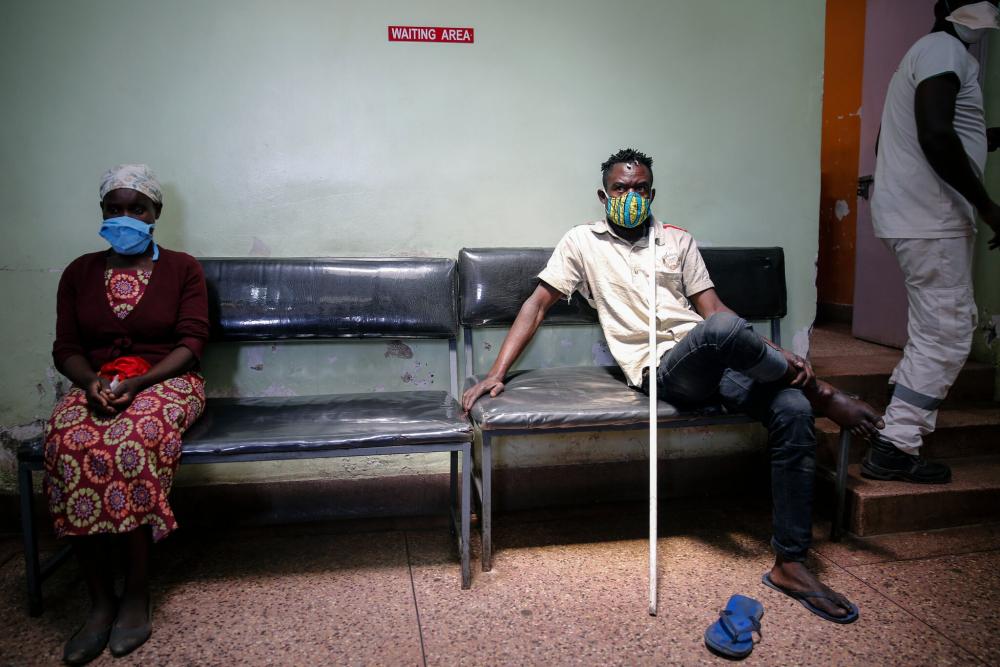
With most private clinics closed, patients with H.I.V., TB and malaria have few places to go for the kind of medical care offered at this Doctors Without Borders clinic in Nairobi.Credit...Brian Inganga/Associated Press
If history is any guide, the coronavirus’s impact on the poor will be felt long after the pandemic is over. The socioeconomic crisis in Eastern Europe in the early 1990s, for example, led to the highest rates in the world of a kind of TB that was resistant to multiple drugs, a dubious distinction the region holds even today.
The starting point in this ruinous chain of events is a failure to diagnose: The longer a person goes undiagnosed, and the later treatment begins, the more likely an infectious disease is to spread, sicken and kill.
For malaria, a short delay in diagnosis can swiftly turn fatal, sometimes within just 36 hours of a spiking fever. “It’s one of those diseases where we cannot afford to wait,” Dr. Alonso said.
Apprehensive about malaria’s rise in West Africa, the W.H.O. is now considering giving entire populations antimalarial drugs — a strategy of last resort used during the Ebola epidemic in West Africa and the Boko Haram insurgency.
Across sub-Saharan Africa, fewer women are coming to clinics for H.I.V. diagnosis. A six-month disruption in access to drugs that prevent H.I.V.-positive pregnant women from passing the infection to their babies in utero could increase H.I.V. infections in children by as much as 139 percent in Uganda and 162 percent in Malawi, according to U.N. AIDS.
Diminishing diagnostic capacity may have the greatest effect on TB, leading to dire consequences for households because, like the coronavirus, the bacterium spreads most efficiently in indoor air and among people in close contact.
Each person with TB can spread the disease to another 15 individuals over a year, sharply raising the possibility of people infected while indoors spreading it among their communities once lockdowns end. The prospect is especially worrisome in densely populated places with high rates of TB, such as the favelas of Rio de Janeiro or the townships of South Africa.
“The more you leave undiagnosed and untreated, the more you will have next year and the year after,” said Dr. Lucica Ditiu, who heads the Stop TB Partnership, an international consortium of 1,700 groups fighting the disease.
The infrastructure built to diagnose H.I.V. and TB has been a boon for many countries grappling with the coronavirus. GeneXpert, the tool used to detect genetic material from the TB bacteria and from H.I.V., can also amplify RNA from the coronavirus for diagnosis.
But now most clinics are using the machines only to look for the coronavirus. Prioritizing the coronavirus over TB is “very stupid from a public health perspective,” Dr. Ditiu said. “You should actually be smart and do both.”
In country after country, the pandemic has resulted in sharp drops in diagnoses of TB: a 70 percent decline in Indonesia, 50 percent in Mozambique and South Africa, and 20 percent in China, according to the W.H.O.

Dr. Giorgio Franyuti said many patients with TB at a makeshift hospital in Mexico City were being misdiagnosed with Covid-19.Credit...Meghan Dhaliwal for The New York Times
In late May in Mexico, as coronavirus infections climbed, TB diagnoses recorded by the government fell to 263 cases from 1,097 the same week last year.
Dr. Giorgio Franyuti, the executive director of Medical Impact, an advocacy group based in Mexico, normally works in the country’s remote jungles, diagnosing and treating TB in the Lacandon people. Unable to travel there during the pandemic, he has worked at a makeshift army hospital treating Covid-19 patients in Mexico City.
There, he has seen nine patients with a sputum-filled cough — characteristic of TB — that began months earlier but who were presumed to have Covid-19. The patients later contracted the coronavirus in the hospital and became seriously ill. At least four have died.
“Nobody is testing for TB at any facility,” he said. “The mind of clinicians in Mexico, as well as decision makers, is stuck with Covid-19.”
“TB is the biggest monster of them all. If we’re talking about deaths and pandemics, 10 million cases a year,” he said, Covid doesn’t compare yet to that toll.
India went into lockdown on March 24, and the government directed public hospitals to focus on Covid-19. Many hospitals shuttered outpatient services for other diseases.
The impact on TB diagnoses was immediate: The number of new cases recorded by the Indian government between March 25 and June 19 was 60,486, compared with 179,792 during the same period in 2019.
The pandemic is also shrinking the supply of diagnostic tests for these killers as companies turn to making more expensive tests to detect the coronavirus. Cepheid, the California-based manufacturer of TB diagnostic tests, has pivoted to making tests for the coronavirus. Companies that make diagnostic tests for malaria are doing the same, according to Dr. Catharina Boehme, the chief executive of the Foundation for Innovative New Diagnostics.
Coronavirus tests are much more lucrative, at about $10, compared with 18 cents for a rapid malaria test.
These companies “have tremendous demand for Covid right now,” said Dr. Madhukar Pai, the director of the McGill International TB Centre in Montreal. “I can’t imagine diseases of poverty getting any attention in this space.”
Treatment interruptions

Thomas Wuoto had to borrow H.I.V. medications from his wife and went without any for 10 days during the lockdown in Nairobi, putting him at risk of developing drug resistance. Credit...Khadija Farah for The New York Times
The pandemic has hindered the availability of drugs for H.I.V., TB and malaria worldwide by interrupting supply chains, diverting manufacturing capacity and imposing physical barriers for patients who must travel to distant clinics to pick up the medications.
And these shortages are forcing some patients to ration their medications, endangering their health. In Indonesia, the official policy is to provide a month’s supply of drugs at a time to H.I.V. patients, but antiretroviral therapy has lately been hard to come by outside of Jakarta.
Even in the city, some people are stretching a month’s supply to two, said “Davi” Sepi Maulana Ardiansyah, an activist with the group Inti Muda.
Mr. Ardiansyah has done so himself, although he knows it has jeopardized his well-being. “This pandemic and this unavailability of the medicines is really impacting our mental health and also our health,” he said.
During the lockdown in Nairobi, Thomas Wuoto, who has H.I.V., borrowed antiretroviral pills from his wife, who also is infected. As a volunteer educator for H.I.V., Mr. Wuoto knew only too well that he was risking drug resistance by mixing or skipping medications. When he finally made it to the Mbagathi County Hospital, he had gone 10 days without his H.I.V. medicines, the first time since 2002 that he had missed his therapy.
People with H.I.V. and TB who skip medication are likely to get sicker in the short term. In the long term, there’s an even more worrisome consequence: a rise in drug-resistant forms of these diseases. Already drug-resistant TB is such a threat that patients are closely monitored during treatment — a practice that has mostly been suspended during the pandemic.
According to the W.H.O., at least 121 countries have reported a drop in TB patients visiting clinics since the pandemic began, threatening hard-fought gains.
“This is really difficult to digest,” Dr. Ditiu said. “It took a lot of work to arrive where we are. We were not at the peak of the mountain, but we were away from the base. But then an avalanche came and pushed us back to the bottom.”
The lockdowns in many places were imposed so swiftly that drug stocks were rapidly depleted. Mexico already had expired drugs in its supply, but that problem has been exacerbated by the pandemic, according to Dr. Franyuti.
In Brazil, H.I.V. and TB drugs are purchased and distributed by the ministry of health. But the coronavirus is racing through the country, and distribution of these treatments has become increasingly difficult as health care workers try to cope with the pandemic’s toll.
“It’s a big logistical challenge to have municipalities have higher stock so they can supply,” said Dr. Betina Durovni, a senior scientist at the Fiocruz Foundation, a research institute in Brazil.
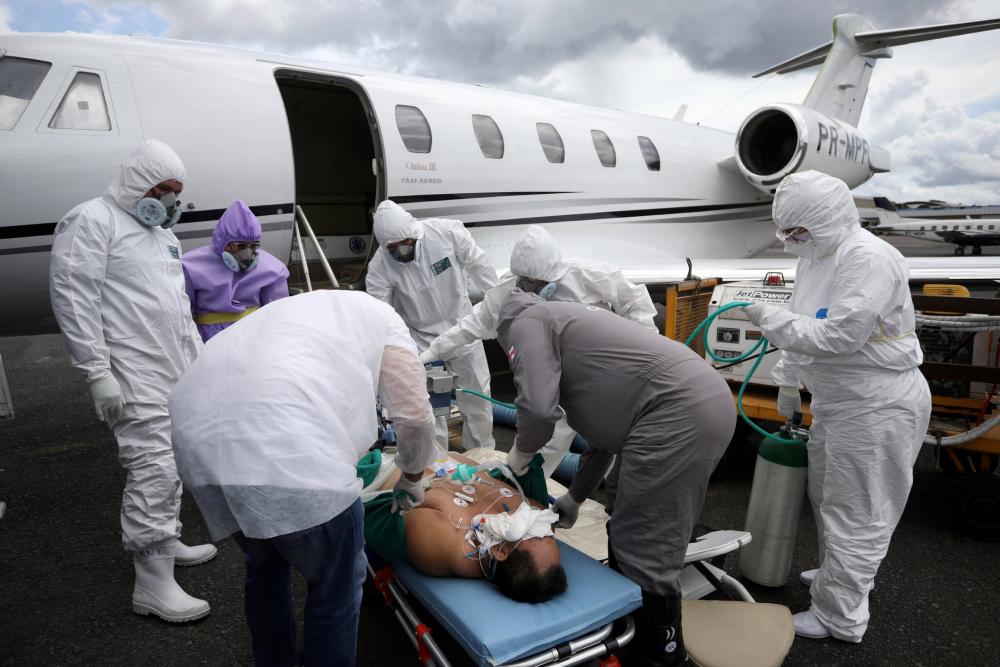
Some coronavirus patients in Tabatinga, Brazil, are airlifted to Manaus, about 1,000 miles away, for treatment, but many more are missed.Credit...Bruno Kelly/Reuters
Even if governments are prepared, with some help from big aid agencies, to buy drugs months in advance, the global supply may soon run out.
The pandemic has severely restricted international transport, hindering the availability not just of chemical ingredients and raw materials, but also of packaging supplies.
“The disruption of supply chains is really something that worries me — for H.I.V., for TB, for malaria,” said Dr. Carlos del Rio, chair of the scientific advisory board of the President’s Emergency Plan for AIDS Relief.
The hype over chloroquine as a potential treatment for the coronavirus has led to hoarding of the drug in some countries like Myanmar, depleting its global stocks.
More than 80 percent of the global supply of antiretroviral drugs comes from just eight Indian companies. The cost of these alone could rise by $225 million per year because of shortfalls in supplies and work force, transport disruptions and currency fluctuations, according to U.N. AIDS.
There is also a real risk that Indian companies will turn to more profitable medicines, or will not be able to meet the global demand because migrant workers have deserted cities as the coronavirus spreads.
The Indian government may even decide not to export TB medicines, saving its supply for its own citizens.
“We’re very dependent on a few key developers or manufacturers for all of the drugs around the world, and that needs to be diversified,” said Dr. Meg Doherty, who directs H.I.V. programs at the W.H.O. “If you had more locally developed drug depots or drug manufacturers, it would be closer to the point of need.”
Aid organizations and governments are trying to mitigate some of the damage by stretching supplies and stockpiling medications. In June, the W.H.O. changed its recommendation for treatment of drug-resistant TB. Instead of 20 months of injections, patients may now take pills for nine to 11 months. The change means patients don’t have to travel to clinics, increasingly closed by lockdowns.
More than half of 144 countries surveyed by the W.H.O. said they have opted to give patients H.I.V. drugs sufficient to last for at least three months — six months, in the case of a few countries like South Sudan — in order to limit their trips to hospitals. But it’s unclear how successful those efforts have been.
In some countries, such as the Philippines, advocacy groups have set up depots for patients to pick up antiretroviral pills or arrange to drop them off at patients’ homes.
In a few nations, like South Africa, most patients already pick up medications from community centers rather than from hospitals, said Dr. Salim S. Abdool Karim, a global health expert in South Africa and the chair of a government advisory committee on Covid-19. “That has been an important advantage in a way.”
‘What are we not doing right?’

The Sally Mugabe Central Hospital in Harare, where Dr. Tapiwa Mungofa works, has closed its outpatient department, where TB and H.I.V. patients received their medications.Credit...Cynthia R. Matonhodze for The New York Times
The pandemic has exposed deep fissures in the health care systems of many countries.
In Zimbabwe, staffs in public hospitals were working reduced shifts even before the pandemic, because the government could not afford to pay their full salaries. Some hospitals like the Sally Mugabe Central Hospital in Harare — which was operating at half capacity because of water shortages and other problems — have since closed their outpatient departments, where TB and H.I.V. patients received their medications.
“Hospitals are functioning in an emergency mode,” said Dr. Tapiwa Mungofa, a physician at the Sally Mugabe Hospital.
The situation is no better in KwaZulu-Natal, which has the highest prevalence of H.I.V. in South Africa. Dr. Zolelwa Sifumba was a teenager when she saw images of skeletal patients dying of AIDS. Over the past few years in KwaZulu-Natal, she is again seeing patients with full-blown AIDS.
“We’re seeing people come in at the stage where they’re kind of on death’s door,” she said. “What are we not doing right?”
Some remote parts of the world are being decimated by the coronavirus — but their very remoteness makes the pandemic’s impact on these other big infectious killers impossible to measure.
The town of Tabatinga in Amazonas, the biggest state in Brazil, is more than 1,000 miles from the closest city with an I.C.U., Manaus. The government has been using airplanes to transport coronavirus patients to Manaus, but many cases are being missed, said Dr. Marcelo Cordeiro-Santos, a researcher at the Tropical Medicine Foundation in Manaus.
Hospitals are giving chloroquine to people with Covid-19, at the recommendation of the Brazilian ministry of health, even though evidence now suggests it does not help and may even be harmful.
Chloroquine is also a crucial malaria medicine, and its indiscriminate use now may lead to resistance to the drug, Dr. Cordeiro-Santos warned — with possibly dire consequences for those infected in the future. But he also said it’s possible that widespread distribution of chloroquine may help protect residents of Amazonas from malaria.
Other experts said they hope the coronavirus pandemic brings some silver linings.
Aid agencies have long recommended that countries buy drugs in bulk and provide several months’ supply at a time to their citizens. Some governments are considering doing so now for H.I.V., according to Dr. Doherty at the W.H.O.
Health care providers are also embracing video and phone calls to counsel and treat patients, which many people find far easier than traveling to distant clinics.
“Sometimes systems are tough to change,” said Dr. del Rio, “but I think there’s nothing better than a crisis to change the system, right?”
Lynsey Chutel contributed reporting from Johannesburg.

Some remote areas in Brazil are being decimated by the coronavirus — but their remoteness makes the impact on other big infectious killers impossible to measure. Credit...Tarso Sarraf/Agence France-Presse — Getty Images
Correction: Aug. 5, 2020
An earlier version of this article referred imprecisely to the region where 90 percent of annual malaria deaths occur. They occur across Sub-Saharan Africa, not only in West Africa.
Apoorva Mandavilli is a reporter for The Times, focusing on science and global health. She is the 2019 winner of the Victor Cohn Prize for Excellence in Medical Science Reporting.
She is the founding editor in chief of Spectrum, an award-winning news site on autism science that grew an audience of millions. She led the team there for 13 years. She joined The Times in May 2020, after two years as a regular contributor.
Apoorva has won numerous awards for her writing. Her work has been published in The Atlantic, Slate and The New Yorker online, and in the anthology ”Best American Science and Nature Writing.”
She co-founded Culture Dish, an organization dedicated to enhancing diversity in science journalism, and was the founding chair of the Diversity Committee for the National Association of Science Writers. Apoorva has a Master of Arts degree in journalism from New York University and a Master of Science degree in biochemistry from the University of Wisconsin-Madison. She is fluent in English, Hindi, Tamil, Telugu and Kannada.


Spread the word